Psoriasis and Atopic Dermatitis: Understanding and Proper Care
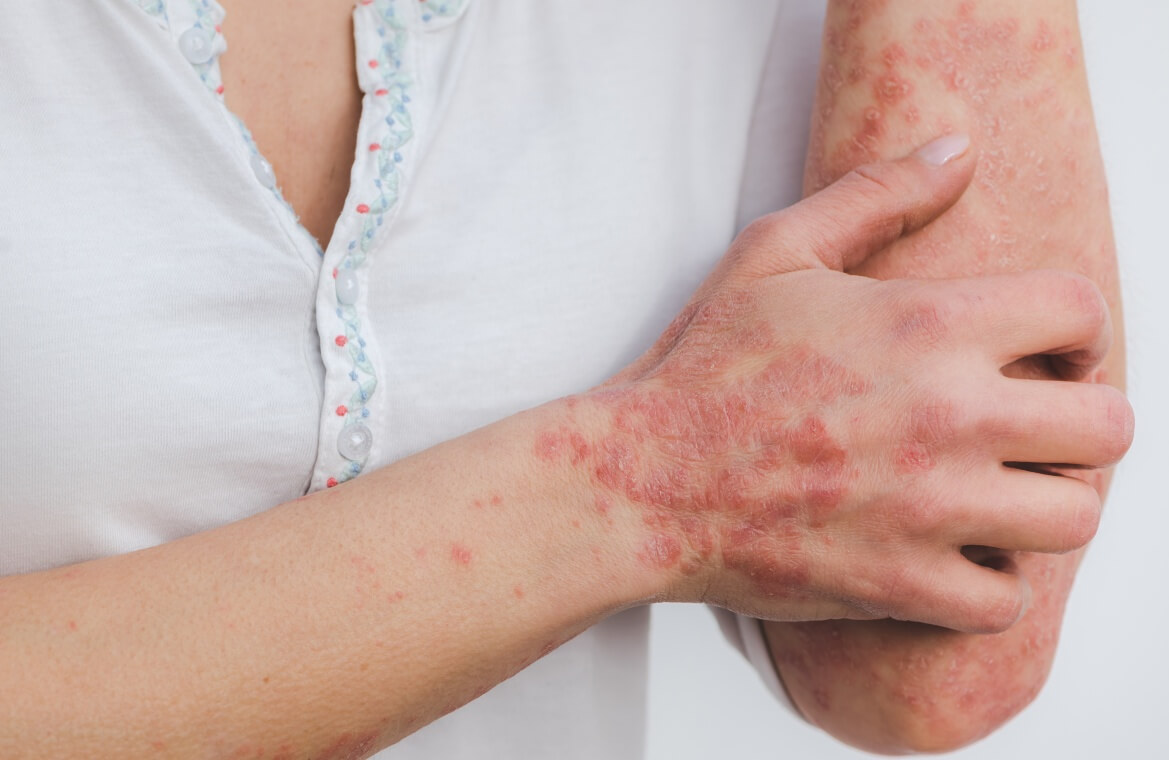
Psoriasis and atopic dermatitis are the two most common chronic immune-mediated skin diseases in the general population. Most of us know a family member, friend, or acquaintance who struggles with skin itching and redness - symptoms that often disrupt daily life, social interactions, work, and intimate relationships.
How to Recognize Psoriasis?
Psoriasis is primarily characterized by redness and scaling of the skin. These plaques most commonly appear on the knees, elbows, lower back, buttocks, hands, scalp, and nails, making them difficult to conceal. Subjective symptoms often include intense itching and burning of the skin and scalp, along with pain associated with psoriatic nails.
Beyond the physical symptoms, sufferers often face significant emotional and social challenges:
- Discomfort when wearing dark clothing due to scales falling from the scalp.
- Carefully choosing outfits to hide affected skin areas.
- Involuntary scratching that leads to bleeding on clothing and bedding.
- Dealing with uncomfortable stares and questions, which can strain social contacts.
Recent medical findings define psoriasis as a systemic disease involving chronic inflammation of the entire body, often linked to conditions such as metabolic syndrome and psychiatric challenges.
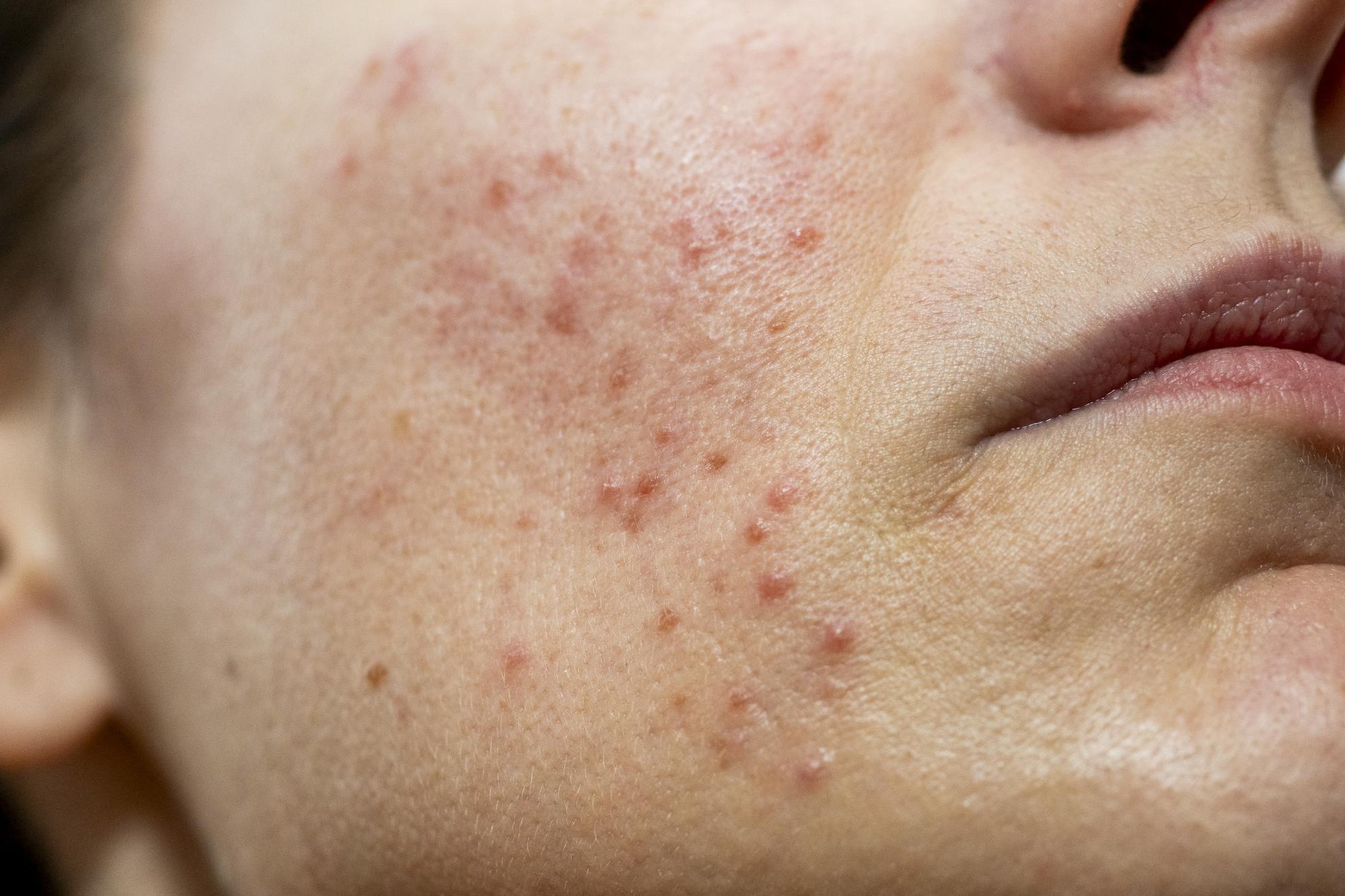
Identifying Atopic Dermatitis
Atopic dermatitis is a chronic, genetically predisposed immune-mediated skin disease. It belongs to the spectrum of atopic conditions, which often include:
- Allergic rhinitis and conjunctivitis
- Allergic bronchitis and asthma
- Food allergies
The main symptoms of atopic dermatitis include redness and dryness during the acute phase, followed by skin thickening (lichenification) in the chronic phase. Changes typically occur on the cheeks and in the folds of the limbs. The hallmark of the disease is intense itching that significantly impairs quality of life. This condition is increasingly common in developed countries, often attributed to the "hygiene theory."
Causes and Triggers: From Genetics to Environment
Both diseases result from a combination of hereditary factors and immune system activation:
Psoriasis: Characterized by accelerated skin cell production and the activation of inflammatory cells. Common triggers include infections, stress, physical injuries, and certain medications.
Atopic Dermatitis: Primarily caused by a damaged skin barrier, which increases sensitivity to allergens and irritants such as perfumes, harsh detergents, wool, cold weather, and dry air.
The Role of Nutrition and Skincare Routine
While diet is not a direct cause, a balanced intake of nutrients can help manage symptoms. Incorporating Omega-3 fatty acids, antioxidants, Zinc, and Vitamin D can support skin health, while regular hydration helps maintain skin elasticity.
When it comes to daily care, consistency is more important than the specific choice of product:
For Psoriasis: Apply creams or lotions 1–3 times daily. Use oil-based cleansers and rich dermocosmetic products containing anti-inflammatory herbal ingredients or urea. Oil baths can help gently remove scales, allowing topical therapies to work more effectively.
For Atopic Dermatitis: Focus on restoring the skin barrier using emollients and moisturizing creams. Avoid irritants like wool and synthetics, and opt for hypoallergenic detergents. For infants, oil baths that do not require rinsing are highly recommended.
Modern Treatments and Disease Control
Traditional topical therapies include corticosteroids, keratolytic agents, and Vitamin D analogs. For moderate to severe cases, systemic therapy and biological drugs have revolutionized treatment outcomes. For atopic dermatitis, non-hormonal PDE4 inhibitors and JAK inhibitors are now available for more severe forms of the disease.
When to Consult a Dermatologist?
If symptoms persist despite proper care for 2–3 months, or if you notice painful plaques, fever, or signs of skin infection, it is time to seek professional help. Early diagnosis and a personalized treatment plan are essential to prevent complications and improve overall well-being.
Final Advice
Managing chronic skin conditions requires patience and a multidisciplinary approach. Keeping a food diary can help identify personal triggers, while stress management techniques like yoga and meditation can reduce the frequency of flare-ups. Remember, while these conditions cannot be fully cured, they can be successfully managed, allowing you to lead a comfortable and active life.

About the author
Iva Blajić
Associate Professor, PhD,Specialist in Dermatology
Iva Blajić graduated in 2006 from the University of Zagreb School of Medicine, where she defended her doctoral dissertation in 2017 entitled Quality of Life and Psychiatric Comorbidity in Dermatovenereology Patients.
After completing her mandatory medical internship, she has been employed since 2007 at the Clinic for Skin and Venereal Diseases, University Hospital Centre Sestre milosrdnice, initially as a research assistant on the Ministry of Science, Education and Sports research project Psychological Status of Patients with Malignant Skin Diseases and Other Dermatoses, and subsequently as a resident in dermatology and venereology.
Since 2016, she has been working as a specialist in dermatology and venereology at the same clinic, with a narrower field of practice in inflammatory-mediated skin diseases and pediatric dermatology. She completed training in pediatric dermatology in London and Padua. She is currently undergoing subspecialization in pediatric dermatology. She participates in numerous clinical trials related to inflammatory skin diseases and is the author and co-author of scientific articles and books.