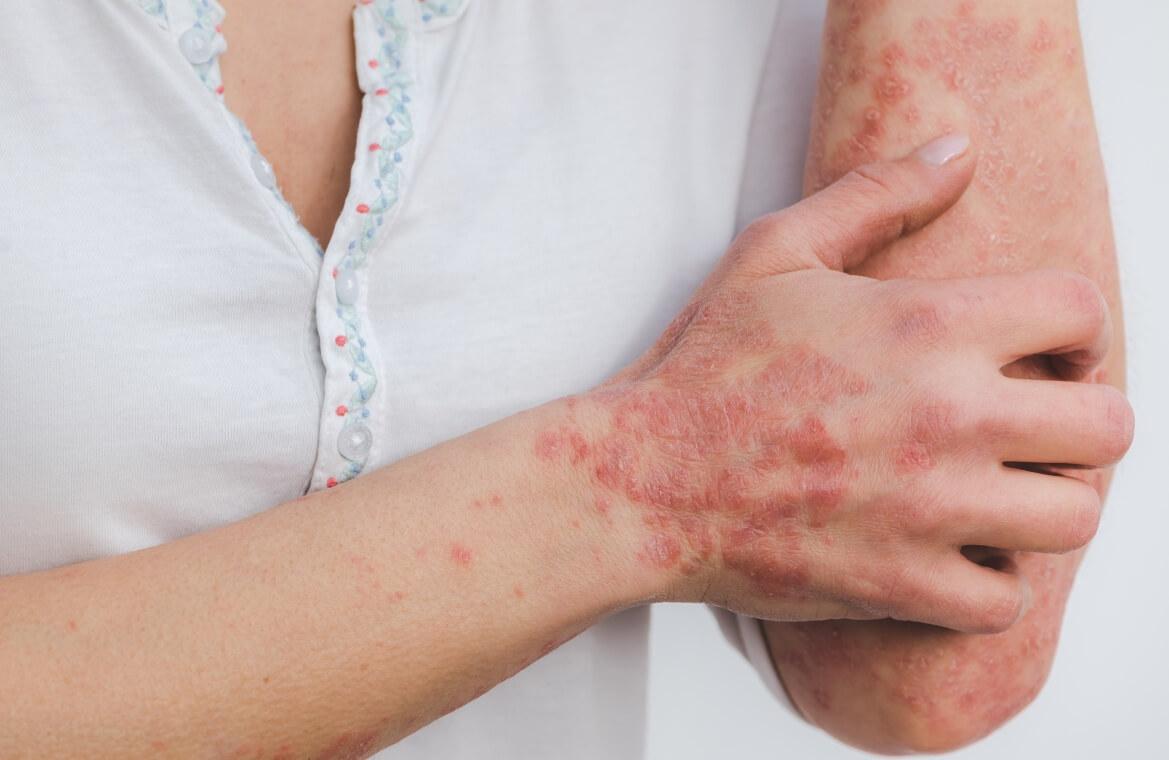
Acne at every age with causes and dermatologist tips for proper care
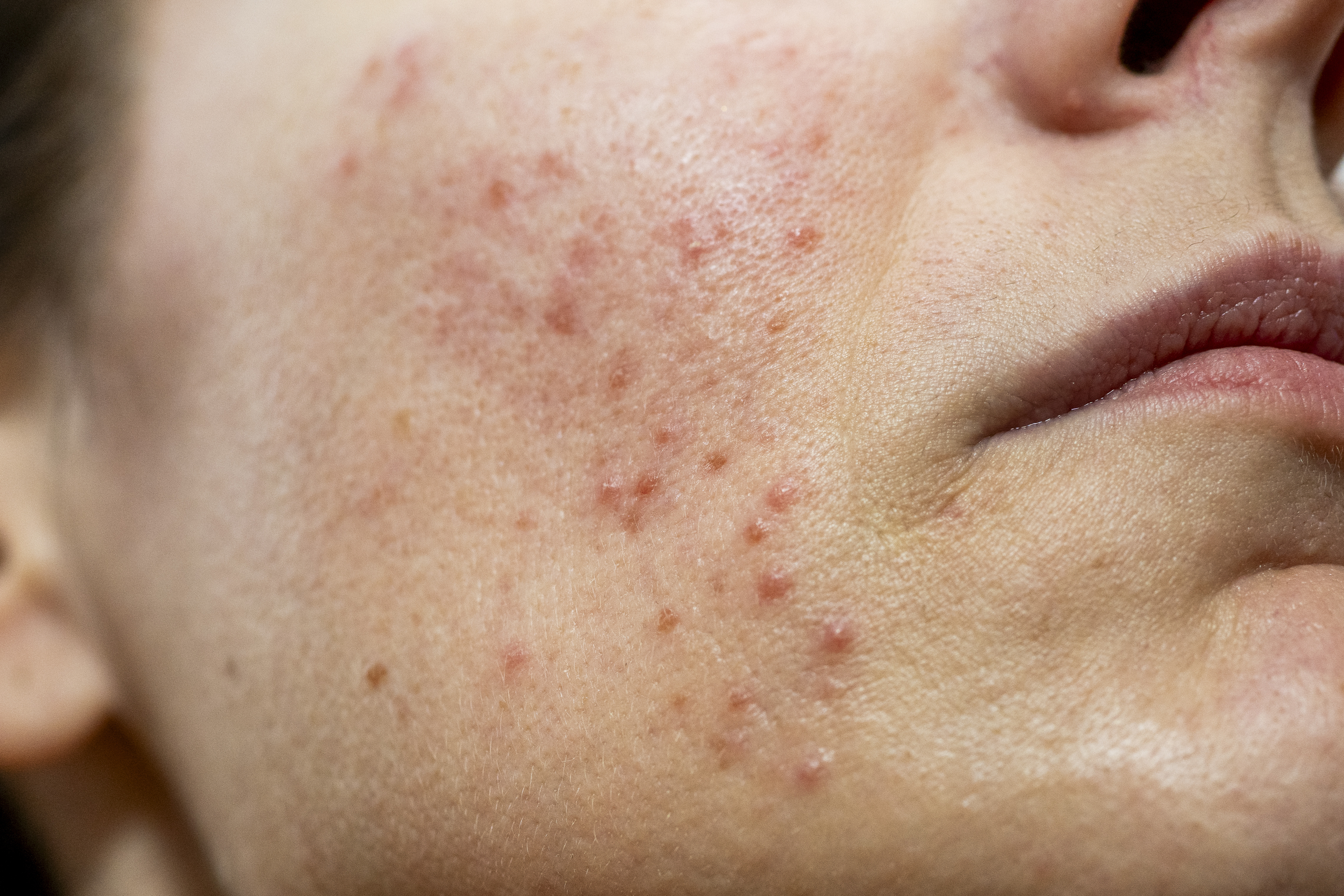
Acne is one of the most common skin conditions. While typically associated with puberty, it can appear at any stage of life—from infancy and childhood to adulthood. A common misconception is that acne is reserved strictly for teenagers and is merely a passing phase that doesn’t require treatment. Adults often advise patience, suggesting one should simply wait for the "hormonal storm" to pass. However, with today’s extensive scientific knowledge and effective therapeutic options, the best course of action is to seek professional advice and an examination by a dermatologist.
What exactly is acne? Acne is a disease of the sebaceous (oil) glands in the skin, which are connected to hair follicles. Its primary characteristic is the comedone (blackhead or whitehead). Beyond comedones, acne is marked by red papules, which may be filled with yellow fluid (pustules), deep subcutaneous nodes, and scarring. Depending on which symptoms prevail, acne is categorized into forms ranging from mild to severe.
Three main reasons why acne develops:
Genetics: We inherit these from our parents, and we cannot change them. What is inherited is a disordered structure of the sebaceous gland ducts. When these ducts become clogged with oil (sebum), a comedone forms—either an "open" one (blackhead) or a "closed" white one that looks like a small, skin-colored cyst.
Hormones: Specifically androgens (male sex hormones), which are present in both men and women and produced in the adrenal glands. These hormones stimulate the sebaceous glands to produce oil. Acne can appear on any area of the skin rich in these glands, predominantly the face (the "T-zone," between the nose and cheeks, and the chin), as well as the chest, shoulders, and upper back.
Note on infants: Newborns receive hormones from the mother via the placenta and can develop neonatal acne, often traditionally referred to as "maternal clearing."
Puberty: As hormone production surges, acne often appears before a girl’s first menstruation. In cases of hormonal imbalance (often reflected in irregular cycles), acne may manifest more severely on the face and torso.
Inflammation: This occurs within the sebaceous duct, aided by skin bacteria that are normal inhabitants of the human skin flora. Numerous inflammatory cells and molecules participate in this process, which is why acne is classified as an inflammatory skin disease. The most feared outcome of this inflammation is scarring. Picking or squeezing acne further intensifies inflammation and increases the likelihood of permanent scars. Therefore, regular cleansing and proper skincare are essential.
Practical Dermatologist Tips for Effective Acne Control
Acne in Puberty – Causes and Care
During puberty, sudden hormonal shifts cause increased sebum production, leading to clogged pores and comedones. If inflammation is triggered, papules and pustules appear. Regardless of severity, a consistent routine is vital.

Tips for Teens and Parents:
Wash your face twice a day with a mild, alcohol-free, and sulfate-free cleanser (gel or cream).
Use lightweight, non-comedogenic moisturizers specifically formulated for oily and acne-prone skin.
Avoid harsh scrubbing and the excessive use of too many dermo-cosmetic products at once.
Do not squeeze pimples – this prevents the spread of infection and scarring.
Seek professional guidance if routine care isn't enough. A dermatologist can prescribe topical treatments (benzoyl peroxide, salicylic acid, retinoids) or systemic treatments (antibiotics or isotretinoin).
Bonus Tip: Monitor diet—excessive sweets, fast food, and high cow’s milk consumption can worsen or trigger breakouts.
Hormonal Adult Acne – When Puberty Ends, but Acne Stays
Adults, especially women, increasingly face acne on the lower third of the face, jawline, and neck. Often, these individuals dealt with acne in their youth or have irregular cycles (sometimes linked to PCOS). Factors like heavy cosmetics, unhealthy lifestyle, metabolic syndrome, or certain medications (corticosteroids, chemotherapy, or psychiatric drugs) contribute to adult acne.
Practical Tips for Adults:
Establish a solid routine: Mild cleanser, light hydration, and SPF protection every morning.
Choose "oil-free" and non-comedogenic makeup.
Reduce stress through relaxation techniques, exercise, and quality sleep.
Track your menstrual cycle and visit a gynecologist if cycles are irregular.
Adjust your diet: Reduce dairy and high-glycemic foods if you notice flare-ups.
Manage weight and stay active—even small daily movements help.
Bonus Tip: If you frequently experience painful, deep acne or scarring after age 25, see a dermatologist; systemic therapy can prevent long-term complications.
Case Study: Ana (28) sought help for acne on her chin and neck. Examination revealed that stress, fast-food habits, and irregular sleep were the main triggers. By introducing a retinoid-based routine, lightweight hydration, and better sleep hygiene, her skin significantly improved within three months.
Acne After 40 – Challenges of Mature Skin
Though less common, acne can appear in one’s 40s and 50s. At this stage, skin is thinner and more sensitive. Hormonal changes (perimenopause and menopause) are often the cause. Sun damage also plays a role, as UV exposure can be comedogenic, leading to "sun-induced" comedones, brown spots, and broken capillaries.

Tips for Mature Skin:
Cleanse gently using micellar water or cleansing creams.
Boost hydration with products containing hyaluronic acid, ceramides, and niacinamide.
Use mild exfoliants, such as enzymatic peels or mandelic acid.
Avoid heavy, oil-based products and aggressive treatments.
Prioritize sun protection: Use SPF 50 and wear a hat.
Bonus Tip: Always check for underlying health or hormonal shifts when acne appears at this age.
Diet, Environment, and Habits
Diet: Research shows that dairy, sugars, and high-glycemic foods can be triggers. Conversely, a diet rich in omega-3 fatty acids, zinc, and vitamins can help. Keeping a "skin and food diary" can help uncover unexpected links.
Environment: Pollution and contact with objects like phones or masks can worsen skin health. Clean your phone regularly, change pillowcases at least once a week, and avoid touching your face with unwashed hands.
When to See a Dermatologist?
If there is no improvement after 2–3 months of proper care, consult a specialist. Pay close attention to painful subcutaneous lumps, acne spreading to the neck and back, or the onset of scarring. Early intervention improves quality of life and prevents permanent damage.
Top 5 Dermatologist Tips for Acne Control:
Wash your face with a mild cleanser twice daily.
Use lightweight, non-comedogenic moisturizers.
Do not squeeze or pick at pimples.
Always apply SPF protection.
Seek professional help if you are unsatisfied with your skin's progress.
Healthier skin through patience and knowledge. Acne is not a sign of poor hygiene, nor is it limited to one age group. Timely expert advice, tailored care, and healthy habits are the best investments in your health and self-confidence.

About the author
Iva Blajić
Associate Professor, PhD,Specialist in Dermatology
Iva Blajić graduated in 2006 from the University of Zagreb School of Medicine, where she defended her doctoral dissertation in 2017 entitled Quality of Life and Psychiatric Comorbidity in Dermatovenereology Patients.
After completing her mandatory medical internship, she has been employed since 2007 at the Clinic for Skin and Venereal Diseases, University Hospital Centre Sestre milosrdnice, initially as a research assistant on the Ministry of Science, Education and Sports research project Psychological Status of Patients with Malignant Skin Diseases and Other Dermatoses, and subsequently as a resident in dermatology and venereology.
Since 2016, she has been working as a specialist in dermatology and venereology at the same clinic, with a narrower field of practice in inflammatory-mediated skin diseases and pediatric dermatology. She completed training in pediatric dermatology in London and Padua. She is currently undergoing subspecialization in pediatric dermatology. She participates in numerous clinical trials related to inflammatory skin diseases and is the author and co-author of scientific articles and books.